May 26, 2026
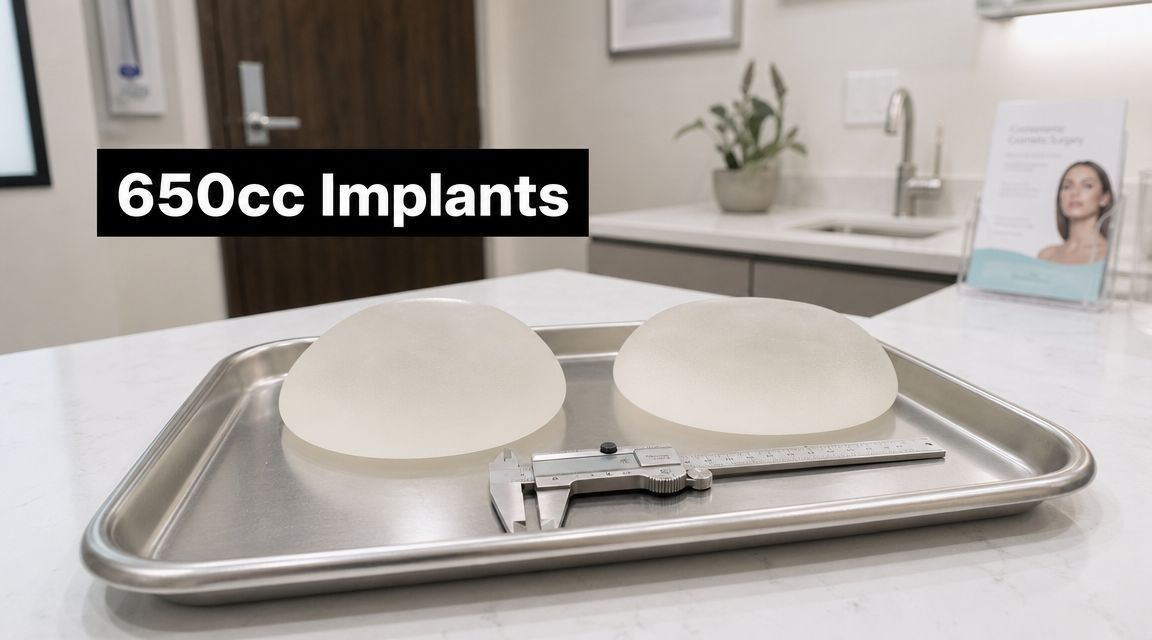
A Patient's Guide to 650cc Breast Implants
Considering 650cc breast implants? Our expert guide covers size, candidacy, results, risks, and what to ask your surgeon on Cape Cod. Get the facts.
Feb 25, 2026

After breast augmentation, one of the most common questions I get is, "How am I supposed to sleep?!" The answer is simple but non-negotiable for the first 4 to 6 weeks: on your back, with your upper body propped up.
Think of this as your secret weapon for a smoother, faster recovery. Getting it right helps manage swelling, protects those delicate incisions, and gives your new implants the best chance to settle perfectly.

After any surgery, your body kicks into high gear to heal. Quality sleep is what fuels that process. It’s when your system can finally focus all its energy on repairing tissue and reducing inflammation.
When you're sleep-deprived, your body pumps out stress hormones like cortisol, which can actually slow down healing and make you feel pain more intensely. So, figuring out how to sleep comfortably isn't just about feeling good—it's about actively protecting your surgical results from any accidental pressure or strain.
Every plastic surgeon will tell you the same thing: for those first few weeks, you absolutely must sleep on your back with your head and shoulders elevated. This isn’t just a suggestion; it’s the gold standard for good reason.
The goal is simple: keep your chest stable, supported, and safe while your body does its healing work. I know it can feel strange, especially if you’re a lifelong side or stomach sleeper, but sticking with it is the single best thing you can do for your final outcome.
For the first 6 to 8 weeks post-op, sleeping on your back with your torso elevated remains crucial. This position prevents you from putting any stress on the new capsule of tissue that naturally forms around your implants, helping them settle into their final position.
Propping yourself up at a 30 to 45-degree angle—either with a wedge pillow or a few strategically stacked bed pillows—can cut down post-operative swelling by as much as 50% in those first few days.
If you want to dive deeper into the recovery process, check out our complete guide on what to expect before and after breast augmentation surgery.

For the first six weeks post-op, sleeping on your back isn't just a helpful tip—it's your most important job. Think of it as a non-negotiable part of the healing process that actively protects your surgical investment.
This position is so crucial because it takes all the pressure off your new incisions and allows your implants to settle naturally and symmetrically into place. Getting this right is fundamental for a beautiful, long-lasting result.
The most immediate benefit you'll notice is a major reduction in swelling. By keeping your upper body elevated at a 30 to 45-degree angle, you're letting gravity do the work. This gentle incline helps drain fluid away from your chest, which makes a huge difference in comfort, especially in the first 48-72 hours.
Beyond managing swelling, back-sleeping is the only way to prevent implant displacement. In the early weeks, the tissue around your implants is incredibly delicate. Any uneven pressure from side or stomach sleeping can push an implant out of its ideal spot. Staying on your back keeps everything stable and centered.
Think of your chest like a delicate sculpture that needs time to set. Back-sleeping is the custom-fit cradle that keeps everything perfectly aligned and undisturbed while the internal healing solidifies.
The first few nights can feel awkward, so preparing your sleep environment ahead of time is a game-changer. You have two fantastic options for getting the elevation and support you need; it really just comes down to personal preference.
Option 1: The Recliner Retreat
Many of my patients swear by sleeping in a recliner for the first week or so. It’s often the simplest solution.
Option 2: The Pillow Fortress
If you’d rather be in your own bed, you can create a setup that’s just as effective.
To keep your spine aligned and stay comfortable all night, the pillow you choose for your head is also key. It’s worth looking into a guide on the best pillows for back sleepers for ideas on what will give your neck the best support.
For lifelong side or stomach sleepers, this is easily the toughest part. My best advice? Start practicing before your surgery.
Try sleeping on your back for a week or two leading up to your procedure. It sounds simple, but getting your body accustomed to the new position ahead of time can dramatically reduce your frustration when you're already sore and exhausted.
Physically blocking yourself in with pillows is your best defense against tossing and turning. Many patients find a U-shaped pregnancy pillow is a fantastic tool; it cradles your entire body and makes rolling over almost impossible.
Remember, this phase is temporary, but its impact on your final result is permanent. Committing to the back-sleeping position is the single most important thing you can do to ensure a smooth recovery and the beautiful outcome you’ve been waiting for.

Getting high-quality, restorative sleep after breast augmentation isn't just about willpower; your environment plays a starring role. One of the best things you can do for yourself is to transform your bedroom into a comfortable and functional recovery space before your surgery day. Think of it as preparing your personal healing haven.
The main goal here is to make sleeping on your back—which is mandatory—not just bearable, but genuinely restful. This means having the right tools on hand to support your body, keep you from accidentally rolling over, and place all your essentials within easy reach to avoid any straining.
You absolutely have to keep your upper body elevated at a 30 to 45-degree angle to manage swelling and take pressure off your incisions. There are two main ways to achieve this, and each has its pros and cons.
The Dedicated Wedge Pillow
From my experience, a firm, high-density foam wedge is often the best choice because of its consistency.
The DIY Pillow Stack
If you'd rather use what you have at home, a well-engineered "pillow fortress" can also do the trick.
For the ultimate in comfort and customized elevation, you might also look into how to get deeper sleep with adjustable beds and Zero Gravity. Being able to adjust your position with the push of a button can be a lifesaver during recovery.
That post-op compression bra isn't just clothing—it’s a critical medical device you'll be living in 24/7. The constant, gentle pressure it provides is absolutely essential for a smooth recovery, especially while you're sleeping.
Wearing a surgical compression bra around the clock is standard practice for at least the first 6 weeks, a protocol recommended by over 90% of board-certified plastic surgeons. This is your number one tool for controlling swelling, which usually peaks around 48-72 hours post-op and can be reduced by 30-40% with proper compression. More importantly, it holds your new implants stable while your body's tissues heal around them. Sleeping without this support too soon can cause the implants to shift, potentially leading to aesthetic problems that might need another procedure to fix.
Think of your compression bra as a 24/7 hug for your chest. It keeps everything snug, supported, and secure, minimizing movement and swelling so your body can focus entirely on healing.
Beyond pillows and your surgical bra, a few other items can make a world of difference in your comfort and your ability to sleep soundly.
U-Shaped Body Pillows
You’ve probably seen these marketed to pregnant women, but they are a recovery superstar. A U-shaped pillow cradles your entire body, supporting your back and hips while creating physical barriers that make it nearly impossible to roll onto your side or stomach in your sleep.
The Fully-Stocked Bedside Table
The last thing you’ll want to be doing is twisting, reaching, or getting out of bed for something in the middle of the night. Before you settle in, make sure your nightstand is armed with everything you could possibly need.
Getting this all set up ahead of time takes so much stress out of the equation. It lets you truly relax, knowing your environment is perfectly arranged to help your body heal.
Pain and tightness are pretty much a given for the first few days and weeks after surgery, but they don't have to ruin your sleep. The trick is to get ahead of the discomfort and keep it there. It's a combination of smart medication timing, some gentle comfort measures, and moving your body correctly. The goal isn't to feel nothing at all, but to keep the discomfort low enough that your body can get the deep, restorative rest it absolutely needs for healing.
Honestly, the biggest mistake I see patients make is waiting until the pain is bad before they take their medication. It's so much harder to chase pain than it is to stay ahead of it.
The most important thing you can do is follow the medication schedule your surgeon gave you. This is not the time to tough it out; staying on top of the pain is what will let you sleep.
A great tip is to time your evening dose strategically. If you know you want to be in bed by 10 PM, take your prescribed pain reliever about 30 to 60 minutes beforehand. This gives it plenty of time to kick in just as you’re settling down, making it much easier to drift off without being distracted by soreness or tightness. For a deeper dive, check out our guide to pain management after surgery.
Medication is your primary tool, but there are other simple things you can do to dial down discomfort and help calm your body before bed. These little tricks can make a surprisingly big difference in soothing inflammation and easing that muscle tightness you’re feeling.
A cool compress can be a lifesaver, but you must get your surgeon’s okay first. A gel pack wrapped in a thin towel and placed on the sides of your breasts (never directly on the incisions) for 15-20 minutes before bed can help numb the area and reduce swelling. Again, never put ice directly on your skin.
Relaxation exercises also work wonders.
The key is to be proactive. When you combine your prescribed medication with these gentle comfort measures, you have a much more powerful toolkit for staying comfortable and getting a peaceful night's sleep.
You'd be surprised how often a sharp, sudden pain comes from simply getting in and out of bed the wrong way. Every time you use your arms to push or pull yourself up, you’re straining the exact muscles that are trying to heal. This is where learning the "log roll" technique becomes non-negotiable.
Getting Into Bed:
Getting Out of Bed:
Mastering this simple move is a game-changer. It prevents unnecessary strain on your incisions and pectoral muscles, which means less pain and better protection for your surgical results.
Your sleep routine is going to change quite a bit as your body heals. I know the first few weeks feel restrictive, but trust me, you won't be stuck sleeping on your back forever. Knowing what to expect week-by-week will help you feel more in control and understand when it’s safe to ease back into your favorite sleeping positions.
The most important thing is to listen to your body and, of course, your surgeon. Trying to switch positions too soon can put a lot of strain on your incisions and mess with how your new implants settle. Think of each phase as giving your body the ideal setup for a great recovery.
This timeline gives you a good visual of what the progression looks like.
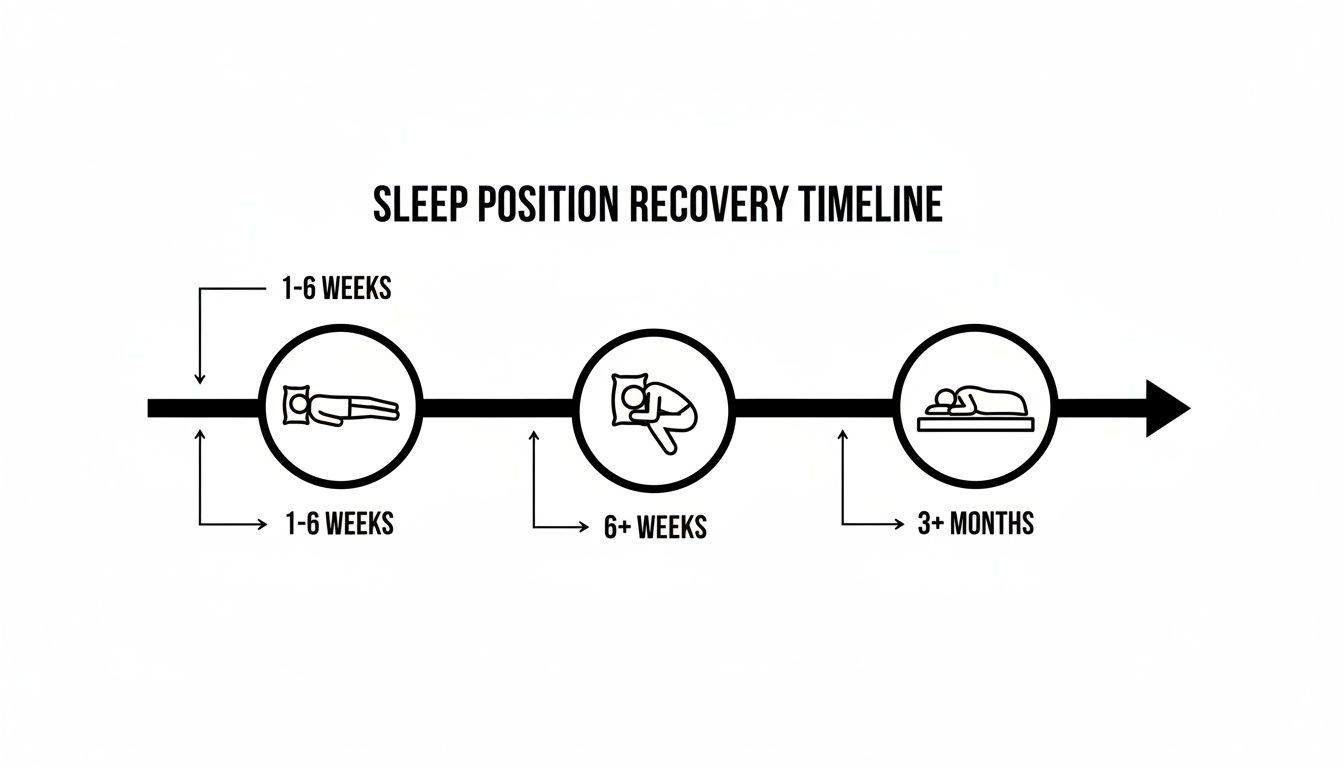
As you can see, those first six weeks are all about sleeping on your back. After that, you can start gradually reintroducing other positions once you’ve hit key healing milestones.
This initial period is without a doubt the most critical part of your recovery. For these first six weeks, sleeping on your back with your upper body elevated is non-negotiable. It's the best way to minimize pressure on your chest, keep swelling down, and let the internal pocket around your implants form and heal properly.
It’s completely normal to feel some new aches during this time, especially in your lower back, from being in one position for so long.
Patience is key here. Your body is doing some incredible healing work, and giving it this stable, pressure-free environment is the single best thing you can do for your long-term results.
After your six-week follow-up appointment, your surgeon will take a close look at how you're healing. If everything is on track, you'll likely get the green light to cautiously start trying to sleep on your side again. For most patients, this is a huge milestone!
But this doesn't mean you can just roll over and fall asleep. Your body is still healing, and your breasts will be sensitive. The transition needs to be slow and supported.
The goal when you start side-sleeping again is to support your breasts, not squish them. Use pillows strategically to keep your chest propped up and stop your top breast from folding over the bottom one.
Start by leaning into a "partial" side-sleeping position, using pillows to prop up your back so you're only at a slight angle. Tuck a soft pillow under your top breast for support and another between your knees to keep your hips and spine happy. If you feel any pulling, sharp pain, or major discomfort, that’s your body’s way of saying it’s not ready. Gently roll back onto your back and try again in another week or so.
Our breast augmentation recovery timeline offers a more detailed look at what to expect at every stage.
Stomach sleeping puts the most direct pressure on your breasts, which is why it's the very last position you should return to. Most surgeons will tell you to wait at least three months—and sometimes longer—before even attempting it. Rushing back to it can actually risk distorting the shape of the implant pocket, which could affect your final look.
When you do finally get clearance from your surgeon, ease into it. Try it for short periods at first and pay close attention to how your body feels. Honestly, some women find that stomach sleeping just isn't comfortable anymore, even months later, and that is perfectly okay.
While you can expect some discomfort during recovery, certain symptoms are not normal and need immediate medical attention. Don't just wait for your next appointment if you experience any of the following, especially if you also have a fever or chills.
Trust your gut. It's always, always better to call your surgeon’s office and get peace of mind than to sit at home and worry. Knowing these warning signs helps you be an active partner in your own safe recovery.
Recovery brings up a lot of questions, and when it comes to something as vital as sleep, it's completely normal to feel a bit anxious. Let's walk through the most common concerns we hear from our patients so you can rest a little easier.
This is, without a doubt, the number one question on everyone's mind. The short answer? Patience is key.
For most patients, we can start talking about side-sleeping around the 4 to 6-week mark. You'll need to get the official green light from your surgeon at a follow-up appointment first. We need that time to ensure the internal pocket that holds your implant has healed properly, without any pressure that could cause things to shift.
Stomach sleeping is a whole different ballgame. It puts the most direct, sustained pressure on your new breasts, so you'll have to wait much longer. The absolute minimum is typically three months, but honestly, many surgeons (myself included) will advise you to wait even longer.
Every patient's healing journey is unique. The timeline is dictated by your body's progress, so always wait for your surgeon to give you their explicit okay before changing your sleep position.
First off, take a deep breath. Don't panic. This is an incredibly common fear, but it's important to know that a brief, accidental roll-over is highly unlikely to cause any real harm.
This is exactly why we recommend building a "pillow fortress" or using a U-shaped body pillow—they make it pretty difficult to roll over in the first place. Plus, your surgical compression bra offers a great deal of protection.
If you do wake up on your side, just gently and slowly move back onto your back. Check in with your body. If you notice any new or sharp pain that doesn't go away, or a sudden change in swelling, that's when you should give our office a call. It's rarely a problem, but we're always here to give you peace of mind.
This one really comes down to personal preference. There’s no right or wrong answer here; what matters is that you can stay comfortably elevated and supported.
The Recliner: A recliner can be a lifesaver, especially during that first week. It locks you into that perfect elevated angle and makes it nearly impossible to roll over. Many patients also find it’s much easier to get up from a recliner without engaging their chest muscles.
The Bed: With the right setup, your own bed can be just as effective and might feel more restful. A good, firm wedge pillow is the perfect base. From there, you can add pillows to support your arms and a small one under your knees to take the pressure off your back.
Here's a tip: Try out your pillow setup in your bed before your surgery day. This little "dress rehearsal" will tell you if you feel secure enough, or if renting or borrowing a recliner might be a better plan for your first few days.
Plan on making that surgical compression bra your best friend 24 hours a day, sleep included, for about four to six weeks. This isn't just a suggestion—it's a critical part of a smooth recovery.
The continuous support from the bra is non-negotiable for two reasons:
After that initial healing phase, your surgeon will likely clear you to transition to a soft, comfortable sports bra (no underwires!) for sleeping for a few more weeks. Always follow the specific timeline your own surgical team gives you, as it’s designed just for you.
At Cape Cod Plastic Surgery, Dr. Fater and our team are here to guide you through every step of your recovery with clear, expert advice. If you're considering breast augmentation, we invite you to schedule a consultation to discuss your goals and create a personalized plan. Learn more about our approach and services at ccplasticsurgery.com.

May 26, 2026
Considering 650cc breast implants? Our expert guide covers size, candidacy, results, risks, and what to ask your surgeon on Cape Cod. Get the facts.

May 25, 2026
Discover active assisted ROM exercises for safe, effective plastic surgery recovery. Our guide explains benefits, techniques, and precautions.

May 24, 2026
Best post op bra - Find the best post-op bra for recovery. Expert guide covers features, sizing & choices for every surgery stage from Cape Cod Plastic